Your brain literally washes itself while you sleep, and keeping a strict bedtime might save your life. For decades, aging was assumed to naturally destroy our ability to get a good night of rest, but a sudden explosion of clinical research has completely rewritten the medical rulebook on how older adults should approach sleep. Scientists are now tracking brain waves, monitoring ambient bedroom temperatures, and deploying global data from hundreds of thousands of participants to understand exactly what happens to the aging mind at night. These eight newly proven breakthroughs give you precise, actionable tools to protect your memory, boost your immune system, and extend your healthspan through better sleep.
The Discovery Deep Dive: 8 Breakthroughs in Senior Sleep Science
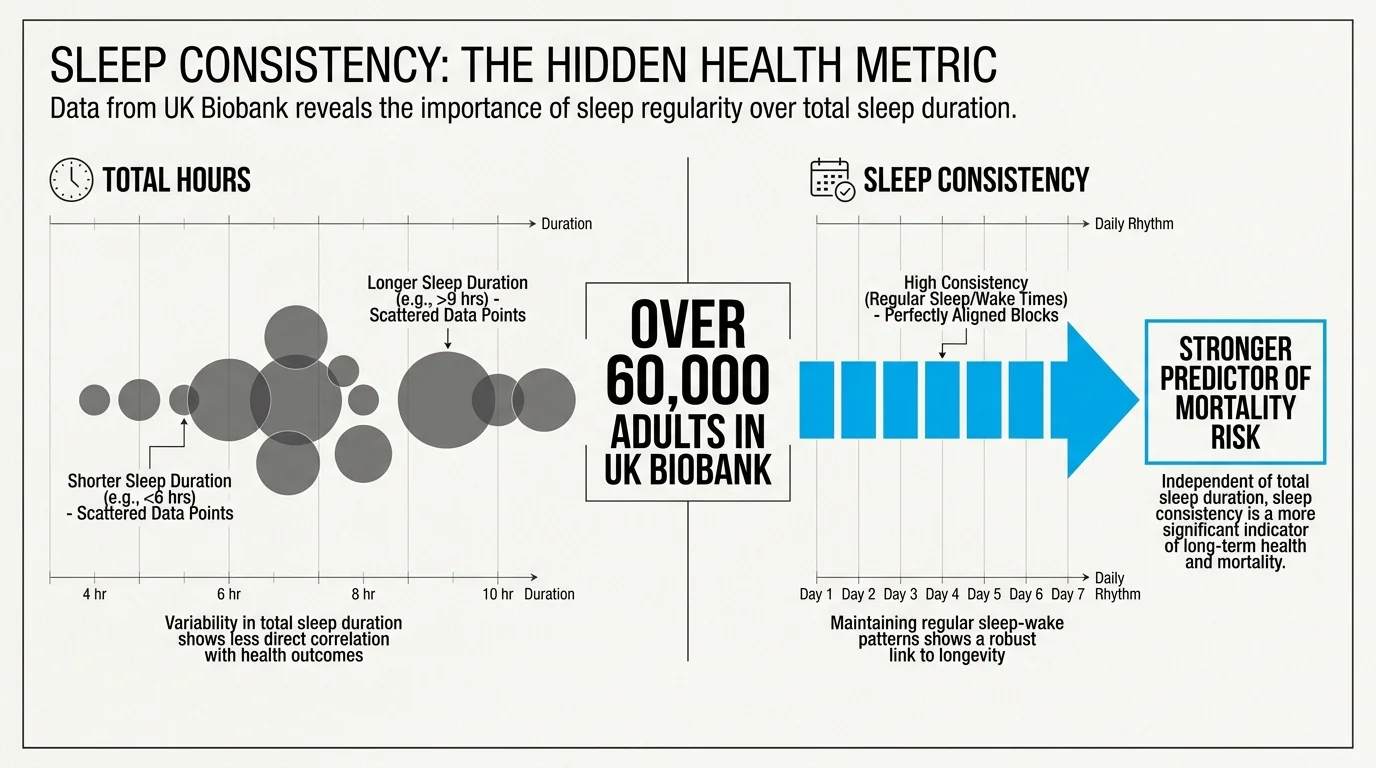
1. Consistency Matters More Than Total Hours
The length of time you sleep might be less important than the exact moment you go to bed. An extensive prospective analysis involving over 60,000 adults in the UK Biobank recently demonstrated that sleep regularity—going to bed and waking up at the exact same time every day—is a significantly stronger predictor of mortality risk than sleep duration. Researchers discovered that individuals with highly irregular sleep-wake patterns faced substantially higher risks of all-cause, cardiovascular, and cancer mortality. Your body relies on a strict circadian rhythm to orchestrate cellular repair; when you constantly shift your sleep schedule, you disrupt these internal clocks. Sticking to a rigorous routine anchors your circadian biology, allowing your body to perform vital maintenance at predictable intervals.
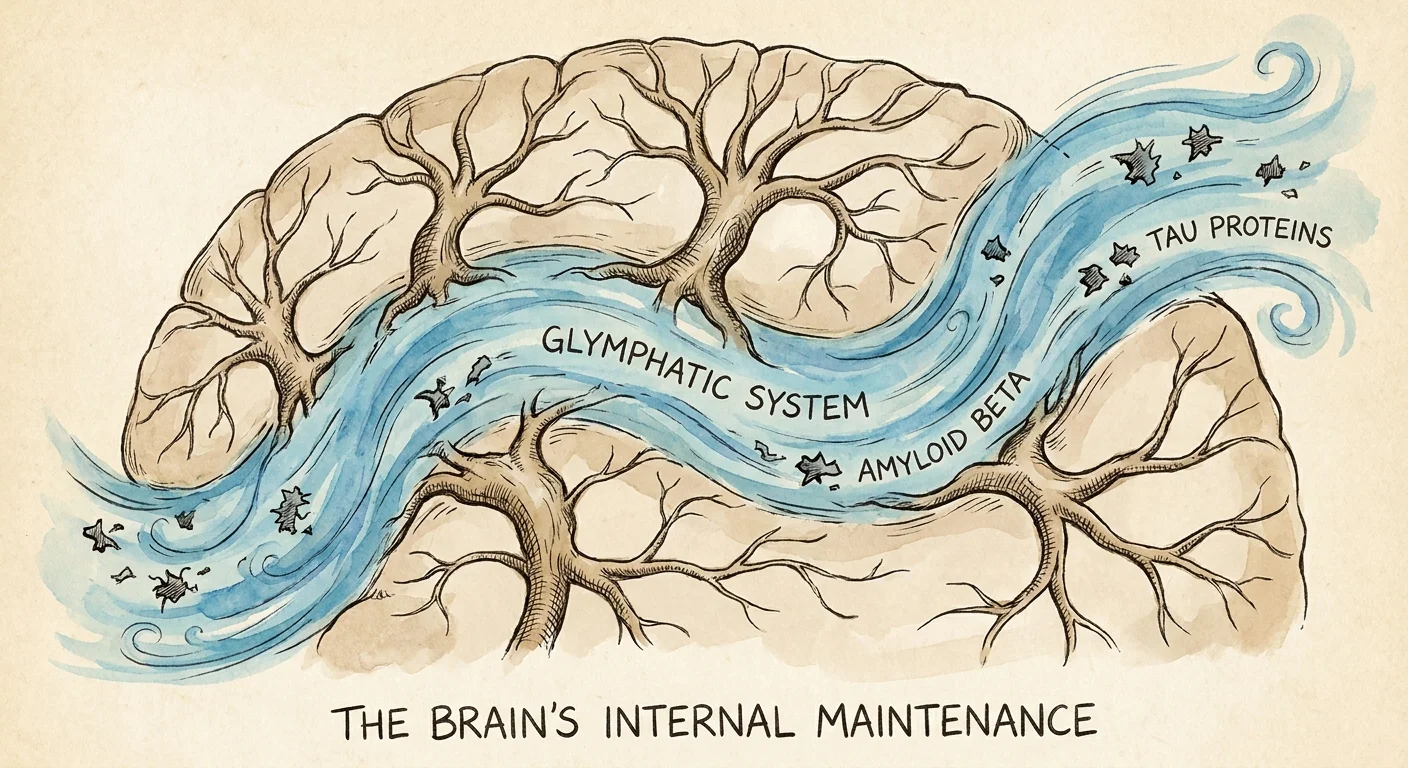
2. Deep Sleep Acts as a Power Washer for Dementia Toxins
Recent clinical trials finally caught the aging brain in the act of cleaning itself. Researchers utilizing advanced cerebrovascular monitoring confirmed that the brain uses the glymphatic system during deep, slow-wave sleep to physically flush out toxic amyloid beta and tau proteins. When older adults entered deep sleep, investigators observed fluid actively sweeping through brain tissue, moving these neurodegenerative proteins into the bloodstream for safe disposal. Conversely, just one night of severe sleep deprivation suppressed this critical clearance mechanism entirely. You can think of deep sleep as an essential overnight power wash for your neurons; without it, cellular waste simply accumulates and damages neural connections over time.

3. The Perfect Bedroom Temperature is Warmer Than You Think
Modern environmental sensors tell a surprising story about bedroom climates. A longitudinal study conducted by researchers at the Harvard Medical School affiliated Marcus Institute tracked community-dwelling seniors in their own homes. They found that older adults sleep most efficiently when their bedroom ambient temperature sits exactly between 68 and 77 degrees Fahrenheit. When nighttime temperatures climbed past this optimal window, sleep efficiency plummeted by as much as ten percent. Because older bodies often struggle with thermoregulation, keeping the bedroom comfortably warm rather than freezing cold prevents the body from expending excess energy to maintain its core temperature, resulting in more restful and uninterrupted slumber.

4. Excessive Morning Naps Serve as an Early Warning System
Taking a short afternoon nap can certainly refresh your mind, but a sudden urge to sleep for long stretches during the day requires medical attention. Utilizing decades of tracking data from older adults, researchers recently pinpointed a dangerous pattern concerning daytime fatigue. Long and frequent morning naps correlate with a sharply increased mortality risk. Taking excessive naps does not merely indicate that you are catching up on lost rest; it often signals an underlying physiological stressor or developing neurodegenerative condition. Scientists noted that each additional hour of daytime napping was associated with a roughly 13 percent higher mortality risk. If you find yourself needing multiple long naps every day to function, your body is likely sounding an alarm about a hidden health issue.

5. Irregular Rhythms Trigger Brain Inflammation
Your immune system extends deep into your brain via specialized cells called microglia, and these microscopic defenders are highly sensitive to your sleep patterns. Recent studies explored what happens to cognitive aging when the sleep-wake cycle becomes chronically misaligned. Investigators discovered that irregular sleep transforms normal, protective microglia into stressed, inflammatory cells. Instead of protecting neural pathways, these stress-primed immune cells begin to release inflammatory chemicals that accelerate cognitive decline. Maintaining a steady rhythm is not just about feeling rested; it is a critical defense mechanism that prevents your brain’s own immune system from turning against healthy tissue.

6. Oversleeping Signals Cognitive Frailty
While sleep deprivation receives most of the media attention, oversleeping presents its own unique dangers for seniors. A comprehensive prospective cohort study tracking older adults revealed a J-shaped curve regarding sleep duration and cognitive frailty—a condition combining physical weakness with mental decline. Participants who slept more than nine hours per night exhibited a significantly higher risk of developing cognitive frailty compared to those who maintained a moderate six to nine hours of rest. Extended sleep duration frequently acts as a biomarker for underlying systemic inflammation, cardiovascular distress, or undiagnosed depression. If you consistently require more than nine hours of sleep to feel functional, you should discuss this pattern with your primary care physician.

7. Deep Sleep Builds a Cognitive Reserve Against Memory Loss
Even if your brain already harbors the toxic proteins associated with Alzheimer’s disease, exceptional sleep quality can protect your active memory. Sleep scientists at the University of California, Berkeley, demonstrated that high volumes of non-REM slow-wave sleep serve as a cognitive reserve factor. Among older adults with identical levels of brain pathology, those who consistently achieved deep sleep exhibited far less active memory decline. Deep sleep fortifies the neural networks that support memory recall, essentially building alternate pathways that bypass damaged tissue. Securing high-quality deep sleep provides a powerful physiological buffer that keeps your mind sharp despite the presence of disease markers.
8. Untreated Apnea Directly Drives Hospitalizations
Gasping for air at night actively pushes you toward the emergency room. Analyzing data from the nationally representative Health and Retirement Study, researchers found that older adults with untreated obstructive sleep apnea face a 21 percent higher probability of future hospitalization. Every time your airway collapses during sleep, your blood oxygen levels plummet, sending shockwaves of stress hormones through your cardiovascular system. This nightly physiological trauma drastically increases your vulnerability to heart failure, strokes, and severe metabolic crashes. Treating sleep apnea with continuous positive airway pressure devices or custom dental appliances immediately removes this cardiovascular burden, keeping you safely at home.

Global Impact: How These Findings Change Aging Worldwide
The intersection of climate change and sleep science has sparked a global public health reckoning. As heat waves become more frequent and severe across Europe, Asia, and the Americas, older adults face unprecedented challenges in maintaining optimal bedroom temperatures. Because science now proves that ambient temperatures exceeding 77 degrees Fahrenheit actively degrade senior sleep architecture, urban planners and policymakers are prioritizing subsidized cooling systems and energy-efficient housing for aging populations.
Furthermore, shifting the medical focus from total sleep duration to sleep regularity requires a massive cultural adjustment. Global healthcare systems are beginning to integrate sleep schedule assessments into routine geriatric care, moving away from simply prescribing sedatives and toward behavioral interventions. In nations with rapidly aging populations, such as Japan and Italy, community health initiatives now emphasize the importance of circadian alignment, encouraging seniors to expose themselves to bright morning sunlight and maintain strict evening routines. This worldwide pivot recognizes that sleep is not a passive state of rest, but an active, highly structured biological intervention that dramatically reduces the global burden of neurodegenerative and cardiovascular diseases.

Expert Voices: What the Scientists Say
Leading neurologists and sleep specialists emphasize that we must stop viewing sleep disturbances as a natural consequence of getting older. Clinical researchers stress that the aging brain does not require less sleep; rather, it often loses the structural ability to generate deep sleep without deliberate behavioral support. Paul Dagum, a pioneer in neurophysiological monitoring, notes that the discovery of the sleep-driven brain clearance system validates the strategy of targeting sleep as a disease-modifying approach for early Alzheimer’s disease. When sleep neurophysiology is disrupted, that vital clearance system simply fails.
Similarly, environmental health researchers advocate for highly personalized sleep environments. Amir Baniassadi, who spearheaded recent investigations into nighttime temperatures, warns against applying blanket advice to all age groups. He points out that older adults possess distinct thermal needs, and optimizing the home environment is a crucial, non-pharmacological lever to enhance sleep quality. Medical professionals increasingly echo these sentiments, urging patients to view their sleep environment and daily schedules as critical components of their preventative healthcare toolkit, right alongside nutrition and physical activity.
Frequently Asked Questions About Senior Sleep
Does waking up in the middle of the night ruin my brain clearance?
Waking up briefly to use the restroom or adjust your blankets does not completely halt your brain’s self-cleaning process. The glymphatic system operates intensely during deep, non-REM sleep, which primarily occurs in the first half of the night. As long as you can comfortably return to sleep and accumulate sufficient slow-wave sleep cycles, minor interruptions will not derail your cellular maintenance. Focus on how refreshed you feel in the morning rather than obsessing over brief awakenings.
Can I offset a bad night of sleep with a long daytime nap?
Long daytime naps cannot replicate the complex biological work performed during overnight deep sleep. Prolonged napping actually reduces your sleep drive, making it much harder to achieve deep sleep the following night. Furthermore, recent data indicates that relying on extensive daytime napping can disrupt your circadian rhythm and is correlated with higher health risks. You are much better off maintaining a consistent bedtime than trying to catch up during the afternoon.
How can I track my sleep regularity at home?
You do not need a laboratory to measure your sleep regularity; you simply need a notebook or a basic smartphone application. By logging the exact time you turn off the lights and the time you get out of bed each morning, you can easily calculate your daily variation. Many modern wearable fitness trackers also monitor sleep-wake times automatically. Your goal should be to keep your sleep and wake times within a strict thirty-minute window every single day, including weekends.
Should I force myself to stay in bed for eight hours?
Lying awake in bed while feeling frustrated actively harms your sleep architecture by associating your mattress with stress. If you cannot fall asleep after twenty minutes, you should get out of bed, move to a dimly lit room, and engage in a calming activity like reading until you feel genuinely tired. Science shows that a slightly shorter, highly consolidated period of deep sleep is far superior to spending eight hours tossing and turning in frustration.
The Forward Look: What Comes Next in Sleep Medicine
The next frontier in sleep science moves beyond simple monitoring and steps directly into active sleep enhancement. Clinical trials are currently underway to test acoustic stimulation devices that play carefully timed bursts of pink noise while older adults sleep. These non-invasive acoustic rhythms are engineered to synchronize with the brain’s slow-wave oscillations, artificially deepening sleep and potentially accelerating the clearance of dementia-linked proteins.
Additionally, chronobiologists are developing precise light therapy protocols tailored specifically for the aging eye, compensating for the cloudy lenses and sluggish retinal receptors that often disrupt circadian signaling in seniors. Instead of developing heavy sedatives, scientists are testing advanced neuro-modulators designed to recreate the exact electrical architecture of youthful deep sleep. As these technologies migrate from university laboratories into consumer bedrooms, you will soon have access to intelligent sleep systems that dynamically adjust temperature, sound, and lighting in real time, actively fighting back against cognitive decline while you dream.