The Hidden Intersection of Aging and a Warming Planet
You step outside to check the mail, and the midday air feels significantly heavier than it did a decade ago. This is not just nostalgia playing tricks on your memory; the global climate is shifting rapidly, and it is reshaping the environment in ways that directly challenge human physiology. While environmental discussions often focus on melting ice caps or endangered wildlife, a pressing medical emergency is unfolding much closer to home. As the planet warms, older adults face a unique and compounding set of health risks. Your body processes heat, air quality, and even hydration differently as you age, making you far more vulnerable to subtle environmental changes.
Understanding these shifts requires moving beyond vague warnings. You need practical, data-backed insights to protect your well-being in a changing world. Environmental scientists and medical researchers are working together to map exactly how shifting weather patterns intersect with the natural aging process. By examining the precise biological mechanisms at play, we can move from anxiety to preparation. Here is a deep dive into the physiological and environmental realities linking climate change to senior health, along with actionable strategies you can employ right now.
Discovery Deep Dive: The Environmental Stressors on Aging Bodies
1. Your Thermoregulation System Loses Its Edge
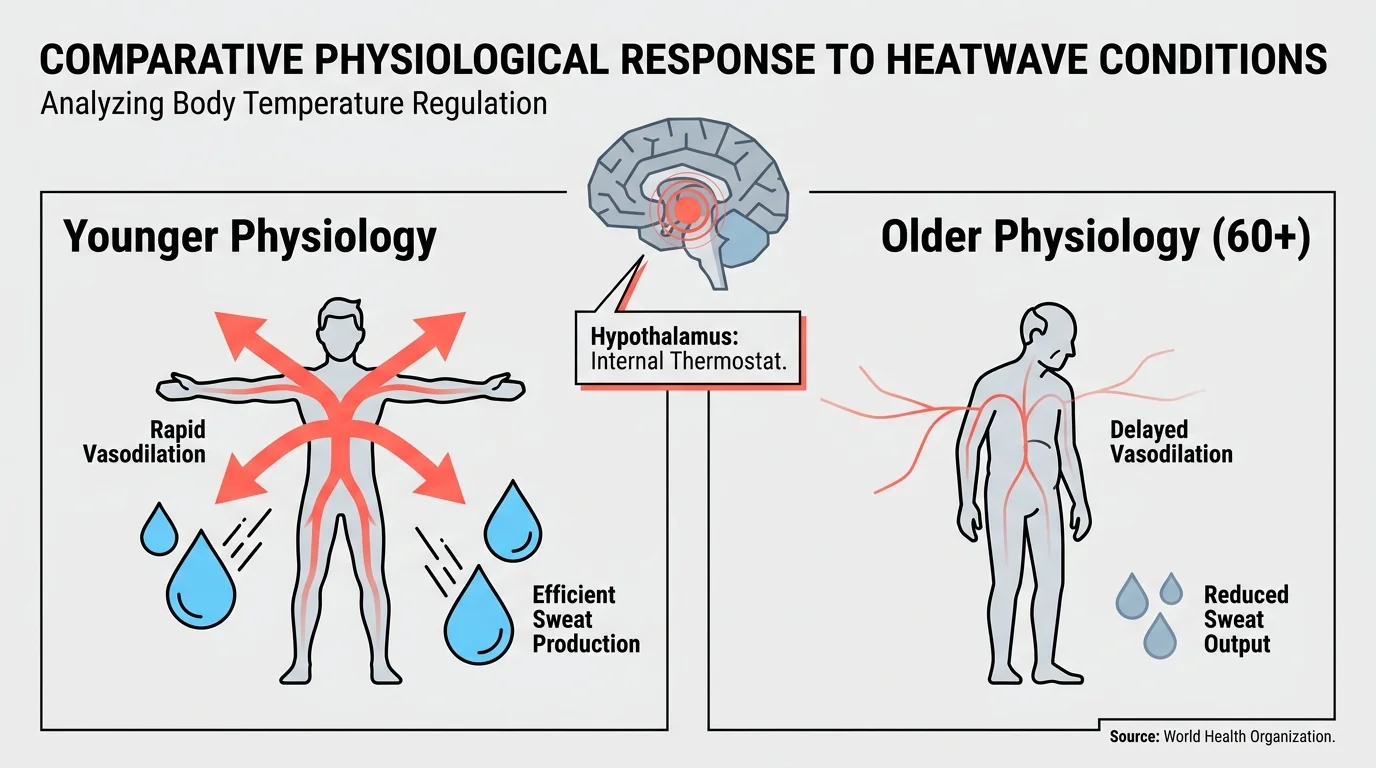
Your body relies on a delicate internal thermostat located in the hypothalamus to maintain a safe core temperature. As you age, this neurological control center becomes less responsive to sudden external temperature spikes. When a severe heatwave strikes, a younger body immediately triggers vasodilation—expanding blood vessels near the skin—and initiates heavy sweating to dissipate heat. In your sixties and beyond, your blood vessels do not dilate as efficiently, and your sweat glands produce significantly less moisture. You might sit in a stifling room and barely register the danger until heat exhaustion sets in.
This physiological lag transforms ordinary summer days into medical hazards. The World Health Organization reports that extreme heat exposure among older adults has skyrocketed over the past two decades, leading to a sharp rise in heat-related cardiovascular mortality. To counteract this, you must rely on external cooling strategies rather than waiting for your body to signal distress. Schedule outdoor activities strictly for the early morning, use air conditioning or robust fans, and drape a damp, cool cloth around your neck to artificially lower your core temperature during peak afternoon heat.
2. Wildfire Smoke Penetrates Deeper into Vulnerable Lungs
Prolonged drought conditions have fueled larger, more intense wildfire seasons across the globe, sending microscopic particulate matter—known as PM2.5—thousands of miles away from the actual flames. These particles are tiny enough to bypass your upper respiratory defenses, embedding themselves deep within your lung tissue and even crossing into your bloodstream. For older adults, lung elasticity naturally diminishes, and the immune system clears out these foreign particles much slower than it once did.
If you manage conditions like chronic obstructive pulmonary disease (COPD), asthma, or even mild heart disease, PM2.5 exposure triggers systemic inflammation that can precipitate acute medical crises. Recent epidemiological research indicates that hospital admissions for older adults spike dramatically in the days following heavy smoke exposure. You can protect your respiratory health by transforming your home into a clean-air sanctuary. Invest in a high-efficiency particulate air (HEPA) purifier, keep your windows closed during smog alerts, and monitor local air quality indices before taking your morning walk.
3. Vector-Borne Diseases Are Invading New Territories
As winters become milder and summers grow longer, ticks and mosquitoes enjoy extended breeding seasons and expanded geographic ranges. Insects that carry diseases like West Nile virus, Lyme disease, and dengue fever are migrating into latitudes and altitudes that previously froze them out. This expansion poses a specific threat to older adults because of a biological process called immunosenescence—the natural, gradual deterioration of the immune system.
When an older adult contracts a vector-borne illness, the resulting infection is often more severe and carries a higher risk of neurological complications. West Nile virus, for example, is statistically more likely to develop into severe encephalitis or meningitis in patients over the age of sixty. You must adapt your outdoor routines to account for these creeping threats. Apply insect repellent containing DEET or picaridin when gardening, wear light-colored long sleeves to easily spot ticks, and eliminate any standing water around your property where mosquitoes might breed.
4. Extreme Weather Severs Access to Essential Medications
Hurricanes, flash floods, and unprecedented winter storms frequently destroy critical infrastructure, disrupting the complex supply chains that deliver medications to local pharmacies. Older adults often rely on a precise daily regimen of prescription drugs to manage blood pressure, diabetes, and heart conditions. When a sudden evacuation order comes through, or a severe storm traps you in your home for a week, missing even a few doses can trigger a cascade of health failures.
Furthermore, navigating a disaster zone makes it incredibly difficult to transfer complex electronic health records or secure emergency refills across state lines. You can mitigate this logistical nightmare by building a robust emergency medical kit. Work with your physician and insurance provider to secure a 30-day backup supply of your most critical prescriptions. Keep these medications in a waterproof bag alongside a printed list of your exact dosages, your doctor’s contact information, and your medical history.
5. Dehydration Risks Multiply as Thirst Mechanisms Fade
The sensation of thirst is actually a late-stage warning sign of dehydration, and unfortunately, this alarm bell becomes muffled as you age. Older adults consistently demonstrate a blunted thirst drive, meaning you can lose a dangerous amount of fluid through insensible perspiration before you ever feel the urge to drink a glass of water. Compounding this issue, aging kidneys slowly lose their maximum ability to concentrate urine, meaning your body wastes more water simply processing daily toxins.
When you combine these internal biological shifts with the rising baseline temperatures of a warming climate, the risk of acute kidney injury escalates rapidly. Dehydration thickens your blood, forces your heart to pump harder, and strains your renal system. You cannot rely on thirst alone to dictate your fluid intake during the warmer months. Establish a rigid hydration schedule—drinking water at set intervals throughout the day—and incorporate water-rich foods like melons, cucumbers, and berries into your daily diet to maintain optimal fluid balance.
6. Climate Anxiety and Isolation Erode Mental Health
Mental health in older populations is profoundly sensitive to environmental instability. When extreme weather forces you to stay locked indoors for days or weeks at a time, the resulting social isolation accelerates cognitive decline and depressive symptoms. You miss out on community gatherings, religious services, and family visits—the very social safety nets that keep the aging mind sharp and engaged.
Additionally, older adults who have lost their homes or communities to floods and fires frequently experience deep trauma and grief. Navigating the chaotic aftermath of a natural disaster requires immense cognitive and emotional energy, which can be overwhelming. To protect your psychological resilience, proactively build a network of digital and phone-based connections. Establish neighborhood check-in systems, so you always have someone to contact—and someone checking on you—when severe weather keeps everyone isolated behind closed doors.
7. Grid Failures Threaten Medical Device Functionality
The modern energy grid is increasingly buckling under the strain of historic heatwaves and violent storms, leading to widespread power outages. For an older adult relying on durable medical equipment, a sudden blackout is not an inconvenience; it is a direct threat to survival. Oxygen concentrators, continuous positive airway pressure (CPAP) machines, motorized wheelchairs, and stairlifts all require an uninterrupted power supply.
Moreover, many vital medications—such as specific types of insulin and biologic treatments for rheumatoid arthritis—must remain strictly refrigerated. When the power fails, these expensive and necessary drugs can spoil within hours. Protect yourself by registering with your local utility company as a vulnerable customer, which often grants you priority during power restoration efforts. Consider investing in uninterruptible power supply (UPS) battery backups for your most critical devices and keep a well-insulated cooler with chemical ice packs ready to preserve your medications.
8. Rising Carbon Dioxide Alters Nutritional Security
Global warming does not just change the weather; it alters the fundamental chemistry of the food you eat. Elevated levels of atmospheric carbon dioxide actually cause staple crops like wheat, rice, and soybeans to grow faster but with significantly lower concentrations of vital nutrients, including protein, zinc, and iron. This phenomenon threatens global food security and poses a distinct risk to older adults, who already face age-related challenges with nutrient absorption.
Deficiencies in iron and zinc impair immune function, slow down wound healing, and contribute to chronic fatigue. If the baseline nutritional value of your food decreases, you must become much more intentional about your diet to compensate. Focus on consuming a diverse array of nutrient-dense whole foods, and consult your healthcare provider about targeted supplementation. Maintaining a high-quality diet is a powerful buffer against the physical stressors introduced by a changing environment.

The Global Impact of a Warming World on Older Adults
The health impacts of a shifting climate do not respect national borders, yet the severity of the crisis varies wildly depending on regional infrastructure and urban planning. In Europe, an aging population combined with historically older architecture has created a uniquely dangerous scenario. Many traditional European homes were built to retain heat during harsh winters and entirely lack modern air conditioning. During the unprecedented heatwaves of 2003 and 2022, tens of thousands of older adults succumbed to the heat inside their own apartments. Since then, cities like Paris and Madrid have heavily invested in retrofitting buildings and establishing community cooling centers.
Conversely, in regions like South Asia and sub-Saharan Africa, older populations face the dual threat of soaring temperatures and fragile power grids. When rolling blackouts strike during a heatwave, relying on electric fans becomes impossible. Urban heat islands—dense metropolitan areas filled with heat-absorbing concrete and asphalt—exacerbate the danger globally. Research published in Nature Climate Change demonstrates that cities with minimal tree canopy coverage record surface temperatures significantly higher than surrounding rural areas, placing older urban residents on the front lines of the climate health crisis.

Voices from the Field: What Experts Say
Public health experts and gerontologists are urgently reshaping their clinical guidelines to account for environmental realities. Medical professionals now view climate change not merely as an ecological issue, but as a dominant social determinant of health. Geriatric specialists note that a patient’s zip code, housing quality, and access to a reliable power grid are just as predictive of their long-term health outcomes as their genetic predispositions.
The Environmental Protection Agency and leading medical societies are aggressively campaigning to educate primary care physicians on the specific signs of heat stress and environmental toxicity in older patients. Experts emphasize that age-related vulnerabilities intersect heavily with socioeconomic status. Older adults living on fixed incomes often hesitate to run their air conditioning due to fear of exorbitant energy bills. Therefore, policy makers are increasingly focused on subsidizing energy costs for seniors, recognizing that a functioning air conditioner is a life-saving medical necessity, not a luxury.
Frequently Asked Questions
How can I protect my refrigerated medications during a power outage?
Keep a dedicated, high-quality cooler stored in an easily accessible location, alongside multiple frozen chemical ice packs in your freezer. If the power goes out, transfer your medications immediately. Do not use regular ice, as melting water can damage the packaging and contaminate your supply. Keep the cooler closed as much as possible to trap the cold air inside.
Are certain prescription medications dangerous during a heatwave?
Yes; many common medications interfere with your body’s ability to handle heat. Diuretics, often prescribed for high blood pressure, increase urination and accelerate dehydration. Beta-blockers reduce blood flow to the skin, limiting your ability to dissipate heat. Never stop taking your medication, but consult your physician about adjusting your dosage or monitoring your fluid intake more aggressively during the summer months.
What is the most effective way to monitor indoor air quality?
You can purchase a dedicated consumer-grade indoor air quality monitor that specifically measures PM2.5 and volatile organic compounds (VOCs). Place the monitor in the room where you spend the most time, typically the bedroom or living room. If the levels rise, activate your HEPA purifier and ensure all windows and external doors are tightly sealed.
How does high humidity change the risk profile for older adults?
Humidity disrupts your body’s primary cooling mechanism: the evaporation of sweat. When the air is heavily saturated with moisture, sweat simply pools on your skin without evaporating, meaning no heat is drawn away from your core. You must pay close attention to the “wet-bulb temperature” or the heat index, which accounts for both heat and humidity. During high humidity, you must rely entirely on air conditioning rather than fans, as blowing hot, wet air over your body provides no physiological relief.
Looking Forward: Innovations in Climate Care
While the statistics may seem daunting, rapid technological and policy innovations are emerging to protect older populations. Urban planners are deploying targeted greening initiatives, planting specific tree species to naturally shade neighborhoods with high concentrations of senior residents. Meanwhile, engineers are developing advanced, reflective “cool roof” materials that drastically lower indoor temperatures without requiring electricity.
In the medical technology sector, wearable health devices are becoming increasingly sophisticated. Smartwatches and biometric rings can now monitor core body temperature, track subtle changes in resting heart rate, and alert you to dangerous drops in blood oxygen levels before you consciously feel ill. The National Institute on Aging continues to fund research exploring how we can fortify human resilience against environmental extremes. Armed with knowledge, modern technology, and proactive community planning, you can successfully adapt your lifestyle to remain healthy, active, and safe in our changing world.